Intellectual and developmental disabilities (IDD) collectively affect one in six individuals in the US, with profound medical, social, and economic consequences.
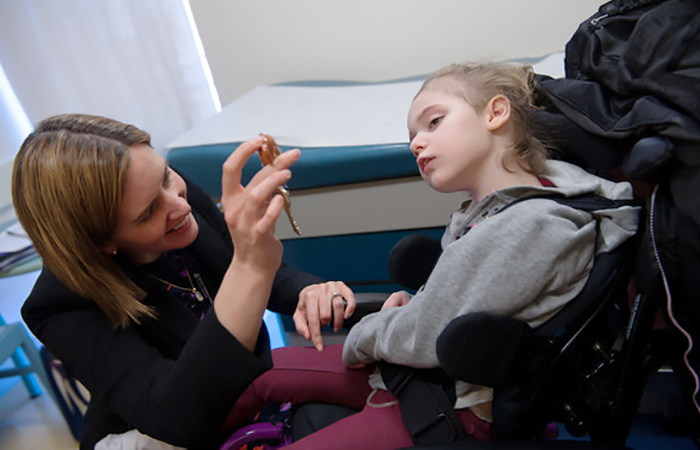

Accelerating cutting-edge research of intellectual and developmental disabilities
The Boston IDDRC accelerates cutting-edge research by immersing investigators in a vibrant scientific community with premier resources within our fully integrated core services, including access to state-of-the-art technologies and consultations with PhD-level core staff. Opportunities for collaboration with top investigators, as well as attendance at select seminars and events, enrich the culture of IDD research and investigation. As a training ground for junior investigators, IDDRC supports the next generation of researchers to ensure the continuation of robust research in the field. Reflecting the capacities of our unique research community, IDDRC Boston focuses its efforts in the areas of Genetics, Genomics and Neuroscience (basic and clinical/translational).
Supporting Investigators
From disease identification through drug discovery
The Center’s fully integrated core structure allows for a seamless movement of the investigator’s research project from one phase to the other. Individual core services can be accessed as well. Guidance and coordination are available to all IDDRC investigators by our superb core leadership and management staff as needed.
Objectives
To stimulate multidisciplinary research across the translational spectrum.
To amplify IDD research through collaborations, especially with other IDDRC and patient-advocacy groups.
To enable research of the highest scientific caliber with state-of-the-art facilities and technologies.
To cultivate the next generation of IDD researchers.
A National Network
The Intellectual and Developmental Disabilities Research Center (IDDRC) at Boston Children’s Hospital (BCH) and Harvard Medical School (HMS) is one of 15 centers supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development, our nation’s first and foremost sustained effort to prevent and treat disabilities through biomedical and behavioral research. We are also a member of the Association of University Centers on Disabilities. IDDRCs contribute to the development and implementation of evidence-based practices by evaluating the effectiveness of biological, biochemical, and behavioral interventions; developing assistive technologies; and advancing prenatal diagnosis and newborn screening.
A Distinguished History
Since its establishment in 1968, IDDRC Boston has benefited from the institutional strengths and infrastructure of a world-class children’s hospital and Harvard’s Longwood Medical Campus. We are an active protagonist of the Boston-Cambridge biotech cluster, serving as the flagship organization for neurodevelopmental disorders. We collaborate in multiple transdisciplinary research collaborations, all aimed at improving the lives of individuals affected with IDD and their families. Our IDDRC provides state-of-the-art support and facilities to a high impact, synergistic program of research and research training in IDD and related areas of brain development.